About Variceal Bleeding
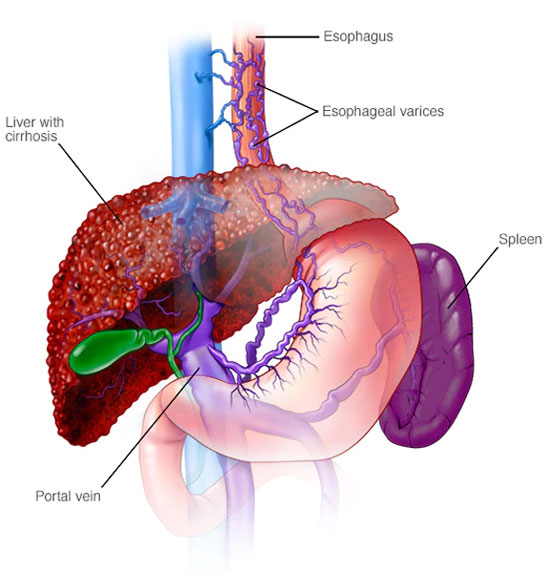
Variceal Bleeding or haemorrhage refers to bleeding from abnormal vascular connections usually found in the oesophagus (esophagus) or stomach. Varices develop when blood pressure in portal veins becomes greater then 10mmHg so blood gets pushed back through alternative routes in order to reach the heart rather than going through the liver. Bleeding occurs when the pressures become even higher. Variceal bleeding is a life-threatening complication of portal hypertension affecting up to 30% of patients with chronic liver disease such as cirrhosis. Of those patients who bleed, nearly half of patients will die and approximately one third with each subsequent bleed. Nearly all patients who have a variceal bleed will have bleeds again in the future, therefore it is very important that these dangerous conditions are identified and treated early to prevent recurrence.
Variceal Bleeding Symptoms
- Vomiting blood
- Black stool
- Tarry stool
- Blood in stool
- Low blood pressure
- Rapid heart rate
- Tarry stool
- Blood in stool
Remember variceal bleeding is an emergency and urgent medical treatment should be sought if you experience the above symptoms. Your doctor will examine you looking for signs of shock (such as heart racing, low blood pressure and cool, clammy skin) due to excessive blood loss. They will also look for signs of liver disease such as clubbing of the fingernails, enlargement of the breasts in males, abnormal spider veins of the skin and an enlarged or nodular liver (felt in the right upper part of the abdomen). The doctor will also insert a gloved finger into the rectum (back passage) to see if there is any blood or dark stools present.
Treatment of Bleeding Varices
Variceal bleeding is a medical emergency so treatment will start immediately. The doctor will determine how severe a patient’s condition is and start resuscitation promptly. It is important that an adequate airway is maintained and oxygen is often given. Occasionally the patient may need to go onto a ventilator to prevent blood entering the lungs. Next, two large drips will be inserted into the patient’s arm and fluids given to help replace the blood volume been lost. Blood transfusion may be needed in severe cases. Once the patient is deemed stable further treatment of the bleeding is required. Drugs such as somatostatin can be given that lower the blood pressure in the portal vessels to help stop the bleeding. Probably the best treatments for bleeding varices are endoscopic procedures. For this a tube with a camera is inserted down the patient’s throat and the varices are either injected with substances that make them clot (sclerotherapy) or have an elastic band tied around them (banding) to stop the bleeding. If these methods fail a balloon may be inserted into the oesophagus or stomach which when inflated provides pressure on the bleeding surface. Sometimes a procedure which inserts a device called a Transjugular intra-hepatic portocaval shunt (TIPS) will be performed if the bleeding does not stop or in patients with recurrent bleeds. This uses x-ray guidance to insert a metal stent (tube) into the liver so blood can drain. Rarely surgery will be needed to tie the vessels feeding the varix or to insert stents at other places. The latter procedures are more permanent and reduce the rates of rebleeding. If you have had a previous bleed or are known to suffer cirrhosis and varices, your doctor can offer other treatments to reduce the chance of future bleeds. The main class of drugs used for this is beta-blockers such as propranolol. These drugs specifically reduce the pressures within the portal vessels. In addition, repeated courses of banding and transjugular intra-hepatic portocaval shunts (TIPS) can be used as long-term measures to prevent recurrence.

